Abstract
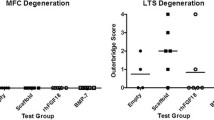
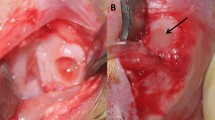
Introduction: In the age of growth factors and gene therapy, the induction of cartilage healing remains an unsolved problem. Even in autologous grafting, one of the preferred methods of treatment for focal osteochondral lesions, chondral integration remains difficult. This study aims to define a possible positive influence of growth factor augmentation on the ingrowth of these transplants. Materials and methods: In an ovine model, questions regarding the healing of osteochondral transplants under the influence of two different growth factors were to be addressed. Two osteochondral autologous transplantations (OAT), one in the weight-bearing surface of each femoral condyle, were performed on the ovine knee using the standard operative protocol. One of the grafts was bathed in augmented PBS containing 50 μg bFGF or bone morphogenetic protein (BMP)-2 directly prior to implantation, while the other condyle served as the control. Two groups, consisting of eight sheep each, were evaluated for each growth factor after 6 months. Results: During the evaluation of all the specimens, neither osteophytes nor synovial changes were observed. The mechanical consistency of the cartilaginous tissue began to reach a level equivalent to the surrounding tissue at 6 months, independent of the use of growth factor. Macroscopically, the superficial border of the transplanted osteochondral plug could easily be outlined in all groups, while the cartilage interface of the bFGF specimens was determined to be less demarcated than the BMP augmented plugs or the controls. Radiographically, a solid osteointegration of the graft could be documented at 6 months in the native and augmented groups. In contrast, integration of the chondral surface of the OAT was not seen macro- or microscopically in any specimen, even though cartilage surfaces remained viable. A firm physical interdigitation of the reconstructed joint surface could not be demonstrated in either of the two augmented groups or the control population. The augmentation with bFGF and BMP-2 stimulated the osseous ingrowth and seems to expedite the remodelling process, but was not able to improve chondral healing. Conclusion: The lack of integration of the cartilaginous portion of the transplanted plugs into the reconstructed joint surface, even following the augmentation with bFGF and BMP-2, does not bode well for the long-term survival of the joint itself.





Similar content being viewed by others
References
Ahmad CS, Cohen ZA, Levine WN, Ateshian GA, Mow VC (2001) Biomechanical and topographic considerations for autologous osteochondral grafting in the knee. Am J Sports Med 29:201–206
Binnet MS, Guerkan I, Karakas A, Yilmaz C, Erekul S, Cetin C (2001) Histopathologic assessment of healed osteochondral fractures. Arthroscopy 17:278–285
Bobic V (1999) The utilisation of osteochondral autologous grafts in the treatment of articular cartilage lesions. Orthopaede 28:19–25
Browne J, Branch TP (2000) Surgical alternatives for treatment of articular cartilage lesions. J Acad Orthop Surg 8:180–189
Cuevas P, Burgos J, Baird A (1988) Basis fibroblast growth factor (FGF) promotes cartilage repair in vivo. Biochem Biophys Res Commun 156:611–618
Duchow J, Hess T, Kohn D (2000) Primary stability of press-fit-implanted osteochondral grafts. Am J Sports Med 28:24–27
Fujimoto E, Ochi M, Kato Y, Mochizuki Y, Sumen Y, Ikuta Y (1999) Beneficial effect of basic fibroblast growth factor on the repair of full thickness defects in rabbit articular cartilage. Arch Orthop Trauma Surg 119:139–145
Fujisato T, Sajiki T, Liu Q, Ikada Y (1996) Effect of basic fibroblast growth factor on cartilage regeneration in chondrocyte-seeded collagen sponges. Biomaterials 17:155–166
Hangody L, Kish G, Kárpáti Z, Szerb I, Udvarhelyi I (1997) Arthroscopic autogenous osteo-chondral mosaicplasty for the treatment of femoral condylar articular defects. Knee Surg Sports Traumatol Arthrosc 5:262–267
Herr G, Schnettler R (1997) Osteoinduktive Aktivitaet von BMP-beschichteten ß-TCP-Keramiken und Charakterisierung der Knochen-Implantat-Grenzschicht. In: Schnettler R, Markgraf E (eds) Knochenersatzmaterialien und Wachstumsfaktoren. Georg Thieme Stuttgart, pp 60–68
Hunter W (1995) The classic: of the structure and disease of articulating cartilages. Clin Orthop 317:3–6
Imhoff AB, Oettl GM, Burkart A, Traub S (1999) Osteochondral autologous transplantation in various joints. Orthopaede 28:33–44
Iwasaki M, Nakahara H, Nakata K, Nakase T, Kimura T, Ono K (1995) Regulation of proliferation and osteochondrogenic differentiation of periosteum-derived cells by transforming growth factor-β and basic fibroblast growth factor. J Bone Joint Surg 77A:543–554
Jackson DW, Lalor PA, Aberman HM, Simon TM (2001) Spontaneous repair of full-thickness defects of articular cartilage in a goat study. J Bone Joint Surg 83A:53–64
Kato Y, Iwamoto M (1990) Fibroblast growth factor is an inhibitor of chondrocyte terminal differentiation. J Biol Chem 265:5903–5909
Kawaguchi H, Kurokawa T, Hanada K, Hiyama Y, Tamura M, Ogata E, Matsumoto T (1994) Stimulation of fracture repair by recombinant human basic fibroblast growth factor in normal and streptozotocin-diabetic rats. Endocrinology 135:774–781
Laprell H, Petersen W (2001) Autologous osteochondral transplantation using the diamond bone-cutting system. Arch Orthop Trauma Surg 121:248–253
Sellers RS, Peluso D, Morris EA (1997) The effect of recombinant human bone morphogenetic protein-2 on the healing of full-thickness defects of articular cartilage. J Bone Joint Surg 79A:1452–1463
Shahgaldi BF, Amis AA, Heatley FW, McDowell J, Bentley G (1991) Repair of cartilage lesions using biological implants. J Bone Joint Surg 73B:57–64
Shapiro F, Koide S, Glimcher MJ (1993) Cell origin and differentiation in the repair of full-thickness defects of articular cartilage. J Bone Joint Surg 75A:532–553
Siebert CH, Miltner O, Schneider U, Wahner T, Koch S, Niedhart C (2001) Healing of osteochondral grafts—an animal study. Z Orthop 139:295–302
Siebert CH, Miltner O, Weber M, Sopka S, Koch S, Niedhart C (2003) Healing of osteochondral grafts in an ovine model under the influence of bFGF. Arthroscopy 19:182–187
Stuetzle H, Hallfeldt K, Keßler S, Schweiberer L (1997) Experimentelle und klinische Ergebnisse mit teildemineralisierter Knochenmatrix. In: Schnettler R, Markgraf E (eds) Knochenersatzmaterialien und Wachstumsfaktoren. Georg Thieme Verlag, Stuttgart, pp 85–89
Trippel SB, Coutts RD, Einhorn TA, Mundy GR, Rosenfeld RG (1996) Growth factors as therapeutic agents. J Bone Joint Surg 78A:1272–1284
Urist MR (1995) The first three decades of bone morphogenetic protein research. Osteologie 4:207–223
Wagner H (1964) Operative Behandlung der Osteochondrosis dissecans des Kniegelenkes. Z Orthop 98:333–355
Wozney JM (1995) The potential role of bone morphogenetic proteins in periodontal reconstruction. J Periodontol 66:506–510
Zellin G, Linde A (2000) Effects of recombinant human fibroblast growth factor 2 on osteogenic cell populations during orthotopic osteogenesis in vivo. Bone 26:161–168
Zlotolow DA, Vaccaro AR, Salamon ML (2000) The role of human bone morphogenetic proteins in spinal fusion. J Am Acad Orthop Surg 8:3–9
Acknowledgement
Financial support was granted by the interdisciplinary centre for clinical research in biomaterials and tissue-material-interaction in implants (BMBF project No. 01 KS 9503/9) of the medical faculty of the RWTH Aachen, Germany and the “Deutsche Arthrose Hilfe”.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Siebert, C.H., Schneider, U., Sopka, S. et al. Ingrowth of osteochondral grafts under the influence of growth factors: 6-month results of an animal study. Arch Orthop Trauma Surg 126, 247–252 (2006). https://doi.org/10.1007/s00402-005-0061-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-005-0061-x