Abstract
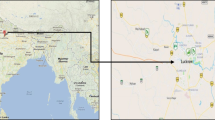
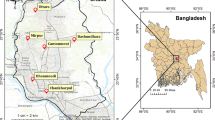
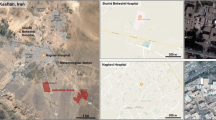
Indoor air quality (IAQ) is a leading apprehension currently especially in the perilous atmosphere, like hospitals. Clean and fresh air is very crucial for the patients and healthcare professionals in the hospitals. Therefore, we examined IAQ indicators (PM1.0, PM2.5, PM10, NO2, CO2, and TVOC) at sixteen locations of three hospitals with an emphasis on seasonal variations, indoor/outdoor correlation, and concomitant toxicity potential (TP) of human exposure between October 2019 and January 2020. For the measurement of trace gases (NO2, CO2, and TVOC), Aeroqual 500 series (New Zealand) sampler was used; particulate matter (PM1.0, PM2.5, and PM10) concentrations and relative humidity (RH) were measured using the IGERESS air quality monitoring device (WP6930S, China). The total average concentration of IAQ indicators were 104.1 ± 67.6 (PM1.0), 137.4 ± 89.2 (PM2.5), and 159.0 ± 103.3 (PM10) μgm−3; 0.11 ± 0.02 (NO2), 1047.1 ± 234.2 (CO2), and 176.5 ± 117.7 (TVOC) ppm. Significant variations of IAQ indicators were observed between different locations of the hospitals. Winter IAQ indicators were much higher than post-monsoon season. Indoor particulate matter (PM) levels were lower than outdoor, but gaseous pollutants were higher in indoor than outdoor except NO2. Indoor TVOC was about two times higher than outdoor and also higher in post-monsoon than winter. A good positive correlation was observed between indoor and outdoor particulate matter during winter. A strong positive correlation was obtained between NO2 and RH with PM in winter. Very high (> 10) indoor toxicity potential (TP) values of PM2.5 and PM10 were determined during winter. Extremely high TP values indicated potential severe health consequences of the healthcare professionals and patients in indoor hospitals’ environment.
Graphical abstract






Similar content being viewed by others
Data Availability
Upon request, authors are able to submit data files.
References
Abdul-Wahab SA, En SCF, Elkamel A, Ahmadi L, Yetilmezsoy K (2015) A review of standards and guidelines set by international bodies for the parameters of indoor air quality. Atmos Pollut Res 6(5):751–767
Almeida-Silva M, Wolterbeek HT, Almeida SM (2014) Elderly exposure to indoor air pollutants. Atmos Environ 85:54–63
American Society of Heating, Refrigerating, Air-Conditioning Engineers, & American National Standards Institute (2001) Ventilation for acceptable indoor air quality, vol 62. American Society of Heating, Refrigerating and Air-Conditioning Engineers
Ashrae A, Standard, A. S. H. R. A. E (2004) Ventilation for acceptable indoor quality. America Society of heating, refrigerating and air-conditioning engineers Inc., Atlanta, GA vol 62
Ayodele CO, Fakinle BS, Jimoda LA, Sonibare JA (2016) Investigation on the ambient air quality in a hospital environment. Cogent Environ Sci 2(1):1215281
Baurès E, Blanchard O, Mercier F, Surget E, Le Cann P, Rivier A et al (2018) Indoor air quality in two French hospitals: measurement of chemical and microbiological contaminants. Sci Total Environ 642:168–179
Bessonneau V, Mosqueron L, Berrubé A, Mukensturm G, Buffet-Bataillon S, Gangneux JP, Thomas O (2013) VOC contamination in hospital, from stationary sampling of a large panel of compounds, in view of healthcare workers and patients’ exposure assessment. PLoS One 8(2):e55535
Bozkurt Z, Üzmez ÖÖ, Döğeroğlu T, Artun G, Gaga EO (2018) Atmospheric concentrations of SO2, NO2, ozone and VOCs in Düzce, Turkey, using passive air samplers: sources, spatial and seasonal variations and health risk estimation. Atmos Pollut Res 9(6):1146–1156
Chamseddine A, Alameddine I, Hatzopoulou M, El-Fadel M (2019) Seasonal variation of air quality in hospitals with indoor–outdoor correlations. Build Environ 148:689–700
Cheng Y, Ho KF, Lee SC, Law SW (2006) Seasonal and diurnal variations of PM1. 0, PM2. 5 and PM10 in the roadside environment of Hong Kong. China Particuology 4(6):312–315
D’Alessandro D, Fara GM (2017) Hospital environments and epidemiology of healthcare-associated infections. In: Indoor Air Quality in Healthcare Facilities. Springer, Cham, pp 41–52
D’Amico A, Pini A, Zazzini S, D’Alessandro D, Leuzzi G, Currà E (2021) Modelling VOC emissions from building materials for healthy building design. Sustainability 13(1):184
Dai CH, Luo YP, Luo S, Qin PF, Peng H (2014) Correlation analysis of PM2. 5 and NO2 concentrations in city ambient air of Changsha. Adv Mater Res 998:1414–1418
de Blas M, Navazo M, Alonso L, Durana N, Gomez MC, Iza J (2012) Simultaneous indoor and outdoor on-line hourly monitoring of atmospheric volatile organic compounds in an urban building. The role of inside and outside sources. Sci Total Environ 426:327–335
De Brouwere K, Cornelis C, Arvanitis A, Brown T, Crump D, Harrison P, Torfs R (2014) Application of the maximum cumulative ratio (MCR) as a screening tool for the evaluation of mixtures in residential indoor air. Sci Total Environ 479:267–276
Demirel G, Özden Ö, Döğeroğlu T, Gaga EO (2014) Personal exposure of primary school children to BTEX, NO2 and ozone in Eskişehir, Turkey: relationship with indoor/outdoor concentrations and risk assessment. Sci Total Environ 473:537–548
Draxler RR, Hess GD (2004) Description of the HYSPLIT 4 modeling system (NOAA technical memorandum ERL ARL-224). NOAA Air Resources Laboratory, Silver Spring
Galindo N, Varea M, Gil-Moltó J, Yubero E, Nicolás J (2011) The influence of meteorology on particulate matter concentrations at an urban Mediterranean location. Water Air Soil Pollut 215(1-4):365–372
Gulshan T, Ali Z, Zona Z, Ansari B, Ahmad M, Zainab M, Nasir ZA, Colbeck I (2015) State of air quality in and outside of hospital wards in urban centers–a case study in Lahore, Pakistan. Pakistan Agricultural Scientists Forum
Heal MR, Kumar P, Harrison RM (2012) Particles, air quality, policy and health. Chem Soc Rev 41(19):6606–6630
Helmis CG, Tzoutzas J, Flocas HA, Halios CH, Stathopoulou OI, Assimakopoulos VD, Panis V, Apostolatou M, Sgouros G, Adam E (2007) Indoor air quality in a dentistry clinic. Sci Total Environ 377(2-3):349–365
Ho KF, Lee SC, Guo H, Tsai WY (2004) Seasonal and diurnal variations of volatile organic compounds (VOCs) in atmosphere of Hong Kong. Sci Total Environ 322(1-3):155–166
Huang H, Cao JJ, Lee SC, Zou CW, Chen XG, Fan SJ (2007) Spatial variation and relationship of indoor/outdoor PM2. 5 at residential homes in Guangzhou city, China. Aerosol Air Qual Res 7(4):518–530
Jayamurugan R, Kumaravel B, Palanivelraja S, Chockalingam MP (2013) Influence of Temperature, Relative Humidity and Seasonal Variability on Ambient Air Quality in a Coastal Urban Area. Int J Atmos Sci 2013:1–7
Jiang C, Li S, Zhang P, Wang J (2013) Pollution level and seasonal variations of carbonyl compounds, aromatic hydrocarbons and TVOC in a furniture mall in Beijing, China. Build Environ 69:227–232
Jung CC, Wu PC, Tseng CH, Su HJ (2015) Indoor air quality varies with ventilation types and working areas in hospitals. Build Environ 85:190–195
Kalaiarasan M, Balasubramanian R, Cheong KWD, Tham KW (2009) Traffic-generated airborne particles in naturally ventilated multi-storey residential buildings of Singapore: vertical distribution and potential health risks. Build Environ 44(7):1493–1500
Kermani M, Arfaeinia H, Nabizadeh R, Alimohammadi M, Aalamolhoda A (2015) Levels of PM2.5-associated heavy metals in the ambient air of Sina Hospital District, Tehran, Iran. J Air Pollut Health 1(1):1–6 Available at: http://japh.tums.ac.ir/index.php/japh/article/view/3 (Accessed: 4 June 2020)
Kulshrestha A, Satsangi PG, Masih J, Taneja A (2009) Metal concentration of PM2.5 and PM10 particles and seasonal variations in urban and rural environment of Agra, India. Sci Total Environ 407(24):6196–6204
Kulshrestha A, Massey DD, Masi J, Taneja A (2013) Source characterization of trace elements in indoor environments at urban, rural and roadside sites in a semi-arid region of India. Aerosol Air Qual Res 14(6):1738–1751
Latha KM, Badarinath KVS (2005) Seasonal variations of PM10 and PM2.5 particles loading over tropical urban environment. Int J Environ Health Res 15(1):63–68
Lee A, Sanchez TR, Shahriar MH, Eunus M, Perzanowski M, Graziano J (2015) A cross-sectional study of exhaled carbon monoxide as a biomarker of recent household air pollution exposure. Environ Res 143:107–111
Lü H, Cai QY, Wen S, Chi Y, Guo S, Sheng G, Fu J, Katsoyiannis A (2010) Carbonyl compounds and BTEX in the special rooms of hospital in Guangzhou, China. J Hazard Mater 178(1-3):673–679
Massey D, Kulshrestha A, Masih TABEJ (2012) Seasonal trends of PM10, PM5.0, PM2.5 & PM1.0 in indoor and outdoor environments of residential homes located in North-Central India. Build Environ 47:223–231
Massey DD, Habil M, Taneja A (2016) Particles in different indoor microenvironments-its implications on occupants. Build Environ 106:237–244
Mendes A, Bonassi S, Aguiar L, Pereira C, Neves SS, Mendes D, Guimarães L, Moroni R, Teixeira JP (2015) Indoor air quality and thermal comfort in elderly care centers. Urban Clim 14:486–501
Mohammadyan M, Keyvani S, Bahrami A, Yetilmezsoy K, Heibati B, Pollitt KJG (2019) Assessment of indoor air pollution exposure in urban hospital microenvironments. Air Qual Atmos Health 12(2):151–159
Montagna MT, Rutigliano S, Trerotoli P, Napoli C, Apollonio F, D’Amico A, De Giglio O, Diella G, Lopuzzo M, Marzella A, Mascipinto S (2019) Evaluation of air contamination in orthopaedic operating theatres in hospitals in southern Italy: the IMPACT Project. Int J Environ Res Public Health 16(19):3581
Moschandreas DJ, Sofuoglu SC (2004) The indoor environmental index and its relationship with symptoms of office building occupants. J Air Waste Manage Assoc 54(11):1440–1451
Nardini S, Cagnin R, Invernizzi G, Ruprecht A, Boffi R, Formentini S (2004) Indoor particulate matter measurement as a tool in the process of the implementation of smoke-free hospitals. Monaldi Arch Chest Dis 61(3):183–192
Nimlyat PS, Kandar MZ (2015) Appraisal of indoor environmental quality (IEQ) in healthcare facilities: a literature review. Sustain Cities Soc 17:61–68
Nunes RAO, Branco PTBS, A.-ferraz MCM, Martins FG, Sousa SIV (2016) Gaseous pollutants on rural and urban nursery schools in Northern Portugal. Environ Pollut 208:2–15
Oh T, Kim M, Lim J, Kang O, Vidya Shetty K, SankaraRao B, Yoo C, Park JH, Kim JT (2012) A real-time monitoring and assessment method for calculation of total amounts of indoor air pollutants emitted in subway stations. J Air Waste Manage Assoc 62(5):517–526
Peixoto MS, de Oliveira Galvão MF, de Medeiros SRB (2017) Cell death pathways of particulate matter toxicity. Chemosphere 188:32–48
Sacks JD, Stanek LW, Luben TJ, Johns DO, Buckley BJ, Ross M (2011) Particulate matter–induced health effects: who is susceptible? Environ Health Perspect 119(4):446–454
Salam A, Bauer H, Kassin K, Ullah SM, Puxbaum H (2003) Aerosol chemical characteristics of a mega-city in Southeast Asia (Dhaka–Bangladesh). Atmos Environ 37(18):2517–2528
Salam A, Al Mamoon H, Ullah MB, Ullah SM (2012) Measurement of the atmospheric aerosol particle size distribution in a highly polluted mega-city in Southeast Asia (Dhaka-Bangladesh). Atmos Environ 59:338–343
Settimo G, Manigrasso M, Avino P (2020) Indoor air quality: a focus on the European legislation and state-of-the-art research in Italy. Atmosphere 11(4):370
Tiwari S, Chate DM, Pragya P, Ali K, Bisht DS (2012) Variations in mass of the PM10, PM2.5 and PM1.0 during the monsoon and the winter at New Delhi. Aerosol Air Qual Res 12(1):20–29
Wang X, Bi X, Sheng G, Fu J (2006) Hospital indoor PM10/PM2.5 and associated trace elements in Guangzhou, China. Sci Total Environ 366(1):124–135
Wolkoff P (2013) Indoor air pollutants in office environments: assessment of comfort, health, and performance. Int J Hyg Environ Health 216(4):371–394
World Health Organization. Occupational and Environmental Health Team. (2006) . WHO Air quality guidelines for particulate matter, ozone, nitrogen dioxide and sulfur dioxide: global update 2005: summary of risk assessment. World Health Organization. https://apps.who.int/iris/handle/10665/69477
Yang Q, Yuan Q, Li T, Shen H, Zhang L (2017) The relationships between PM2.5 and meteorological factors in China: seasonal and regional variations. Int J Env Res Pub He 14(12):1510
Yurtseven ERAY, Erdogan MS, Ulus TÜMER, Sahin UA, Onat B, Erginoez ETHEM, Vehid S, Koeksal SELÇUK (2012) An assessment of indoor PM2.5 concentrations at a medical faculty in Istanbul, Turkey. Environ Prot Eng 38(1):115–127
Zhang J, Sun Y, Wu F, Sun J, Wang Y (2014) The characteristics, seasonal variation and source apportionment of VOCs at Gongga Mountain, China. Atmos Environ 88:297–305
Acknowledgments
The authors acknowledge the support from Dhaka Medical College and Hospitals (DMCH), Bangabandhu Sheikh Mujib Medical University (BSMMU), and Sonargaon Upazila Hospitals authority for allowing us to conduct sampling in their premises.
Funding
No external financial support was taken for this study on top of the resources of the Department of Chemistry, University of Dhaka, Bangladesh.
Author information
Authors and Affiliations
Contributions
Shahid Uz Zaman: Data collection and initial drafting of the manuscript
Mahbuba Yesmin: Conceptual idea, analyzing data, and editing of the manuscript
Md. Riad Sarkar Pavel: Data collection and initial drafting of the manuscript
Farah Jeba: Editing of the manuscript and data analysis
Abdus Salam: Conceptual idea and editing of the manuscript
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This is not applicable for this manuscript.
Consent for publication
Yes.
Competing interests
The authors declare no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Responsible Editor: Philippe Garrigues
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
• Indoor air quality (IAQ) indicators and toxicity potential were studied in the hospitals.
• Indoor PM2.5 levels exceeded the ambient WHO standard up to 10 times during winter.
• IAQ indicators have significant variations among different locations inside each hospital.
• Strong seasonal variations were observed in both indoor and outdoor environments.
• Toxicity potential values indicated ascetic health consequences on hospital occupants.
Supplementary Information
ESM 1
(DOCX 18.4 kb)
Rights and permissions
About this article
Cite this article
Zaman, S.U., Yesmin, M., Pavel, M.R.S. et al. Indoor air quality indicators and toxicity potential at the hospitals’ environment in Dhaka, Bangladesh. Environ Sci Pollut Res 28, 37727–37740 (2021). https://doi.org/10.1007/s11356-021-13162-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-021-13162-8