Abstract
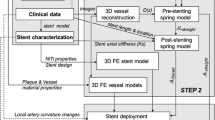
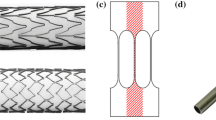
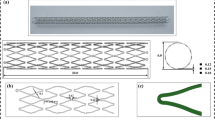
Although the number of fractured stents in the femoro-popliteal district was largely reduced using second-generation devices, remarkable differences still exist among various products. In vitro testing offers a valid tool to comparatively assess the risk of fatigue fracture of different devices. However, there are no standardized methodologies for bench testing under the complex biomechanical environment of the femoro-popliteal district. A computational approach was used in the present study to investigate the fatigue testing conditions adopted in the in vitro studies to increase the understanding of the Nitinol stents fatigue behaviour, by focusing on the role of the stent–wall interaction. The finite element method was used coupled to fatigue analysis to investigate the behaviour of commercial devices during in vitro tests. Two peripheral stents were chosen for the analyses for which conflicting results are found in literature. Stent models were subjected to axial compression and bending either alone in the fully-expanded configuration or after their deployment in a silicone tube resembling the presence of the artery. Results indicate that the two testing conditions investigated produce quite a different fatigue behaviour both in terms of constant-life diagram and strain distribution in the stents. In particular, the results highlight that oversizing influence the fatigue behaviour of the devices with an effect on both the mean and amplitude values of the strain induced in the stents. Comparison with a fatigue limit typical for Nitinol indicates good agreement with the experimental results and confirms the validity of the adopted methodology. Stent oversizing plays an important role in determining the fatigue response of the devices and cannot be disregarded to assess the fatigue performance of Nitinol stents during in vitro tests. Moreover, the different behaviour found for the two stent models suggests that a careful stent design can improve the fatigue performance of these devices.








Similar content being viewed by others
References
Allie, D. E., C. J. Hebert, and C. M. Walker. Nitinol stent fracture in the SFA. Endovasc. Today 3(7):22–34, 2004.
Arthurs, Z. M., P. D. Bishop, L. E. Feiten, M. J. Eagleton, D. G. Clair, and V. S. Kashyap. Evaluation of peripheral atherosclerosis: a comparative analysis of angiography and intravascular ultrasound imaging. J. Vasc. Surg. 51(4):933–938, 2010.
Bosiers, M., G. Torsello, H. M. Gissler, J. Ruef, S. Müller-Hülsbeck, T. Jahnke, P. Peeters, K. Daenens, J. Lammer, H. Schroë, K. Mathias, R. Koppensteiner, F. Vermassen, and D. Scheinert. Nitinol stent implantation in long superficial femoral artery lesions: 12-month results of the DURABILITY I study. J. Endovasc. Ther. 16(3):261–269, 2009.
Cheng, C. P., N. M. Wilson, R. L. Hallett, R. J. Herfkens, and C. A. Taylor. In vivo MR angiographic quantification of axial and twisting deformations of the superficial femoral artery resulting from maximum hip and knee flexion. J. Vasc. Interv. Radiol. 17(6):979–987, 2006.
Dick, P., H. Wallner, S. Sabeti, C. Loewe, W. Mlekusch, J. Lammer, et al. Balloon angioplasty versus stenting with Nitinol stents in intermediate length superficial femoral artery lesions. Catheter. Cardiovasc. Interv. 74:1090–1095, 2009.
Duda, S. H., M. Bosiers, J. Lammer, D. Scheinert, T. Zeller, V. Oliva, A. Tielbeek, J. Anderson, B. Wiesinger, G. Tepe, A. Lansky, M. R. Jaff, C. Mudde, H. Tielemans, and J. P. Beregi. Drug-eluting and bare nitinol stents for the treatment of atherosclerotic lesions in the superficial femoral artery: long-term results from the SIROCCO trial. J. Endovasc. Ther. 13(6):701–710, 2006.
Ganguly, A., J. Simons, A. Schneider, B. Keck, N. R. Bennett, R. J. Herfkens, and R. Fahrig. In-vivo imaging of femoral artery nitinol stents for deformation analysis. J. Vasc. Interv. Radiol. 22(2):244–249, 2011.
Gibbs, J. M., S. P. Costantino, and J. Benenati. Treating the diseased superficial femoral artery. Tech. Vasc. Interv. Radiol. 13:37–42, 2010.
Harvey, S. M. Nitinol stent fatigue in peripheral artery subjected to pulsatile and articulation loading. J. Mater. Eng. Perform. 20(4–5):697–705, 2011.
Iida, O., M. Uematsu, Y. Soga, K. Hirano, K. Suzuki, H. Yokoi, T. Muramatsu, N. Inoue, S. Nanto, and S. Nagata. Timing of the restenosis following nitinol stenting in the superficial femoral artery and the factors associated with early and late restenoses. Catheter. Cardiovasc. Interv. 78(4):611–617, 2011.
Klein, A. J., S. J. Chen, J. C. Messenger, A. R. Hansgen, M. E. Plomondon, J. D. Carroll, and I. P. Casserly. Quantitative assessment of the conformational change in the femoropopliteal artery with the leg movement. Catheter. Cardiovasc. Interv. 74(5):787–798, 2009.
Kleinstreuer, C., Z. Li, C. A. Basciano, S. Seelecke, and M. A. Farber. Computational mechanics of Nitinol stent grafts. J. Biomech. 41:2370–2378, 2008.
Krankenberg, H., M. Schlüter, H. Steinkamp, K. Bürgelin, D. Scheinert, K. L. Schulte, E. Minar, P. Peeters, M. Bosiers, G. Tepe, B. Reimers, F. Mahler, T. Tübler, and T. Zeller. Nitinol stent implantation versus percutaneous transluminal angioplasty in superficial femoral artery lesions up to 10 cm in length: the femoral artery stenting trial (FAST). Circulation 116(3):285–292, 2007.
Laird, J. R., B. T. Katzen, D. Scheinert, J. Lammer, J. Carpenter, M. Buchbinder, R. Dave, G. Ansel, A. Lansky, E. Cristea, T. J. Collins, J. Goldstein, and M. R. Jaff. Nitinol stent implantation versus balloon angioplasty for lesions in the superficial femoral artery and proximal popliteal artery. Twelve-month results from the RESILIENT randomized trial. Circ. Cardiovasc. Interv. 3(3):267–276, 2010.
Lownie, S. P., D. M. Pelz, D. H. Lee, S. Men, I. Gulka, and P. Kalapos. Efficacy of treatment of severe carotid bifurcation stenosis by using self-expanding stents without deliberate use of angioplasty balloons. Am. J. Neuroradiol. 26(5):1241–1248, 2005.
Mewissen, M. W. Primary nitinol stenting for femoropopliteal disease. J. Endovasc. Ther. 16(2):1163–1181, 2009.
Müller-Hülsbeck, S., P. J. Schäfer, N. Charalambous, H. Yagi, M. Heller, and T. Jahnke. Comparison of second-generation stents for application in the superficial femoral artery: an in vitro evaluation focusing on stent design. J. Endovasc. Ther. 17(6):767–776, 2010.
Nikanorov, A., H. B. Smouse, K. Osman, M. Bialas, S. Shrivastava, and L. B. Schwartz. Fracture of self-expanding nitinol stents stressed in vitro under simulated intravascular conditions. J. Vasc. Surg. 48(2):435–440, 2008.
Pelton, A. R. Nitinol fatigue: a review of microstructures and mechanism. J. Mater. Eng. Perform. 20(4–5):613–617, 2011.
Pelton, A. R., X. Y. Gong, and T. Duerig. Fatigue testing of diamond-shaped specimens. Proceedings of the International Conference on Shape Memory and Superelastic Technologies. SMST 2003, Pacific Grove, CA, pp. 199–204.
Pelton, A. R., V. Schroeder, M. R. Mitchell, X. Y. Gong, M. Barney, and S. W. Robertson. Fatigue and durability of Nitinol stents. J. Mech. Behav. Biomed. Mater. 1:153–164, 2008.
Petrini, L., W. Wu, E. Dordoni, A. Meoli, F. Migliavacca, and G. Pennati. Fatigue behavior characterization of nitinol for peripheral stents. Funct. Mater. Lett. 2012. doi:10.1142/S1793604712500129.
Saguner, A. M., T. Traupe, L. Räber, N. Hess, Y. Banz, A. R. Saguner, N. Diehm, and O. M. Hess. Oversizing and restenosis with self-expanding stents in iliofemoral arteries. Cardiovasc. Interv. Radiol. 35(4):906–913, 2012.
Saidane, K., S. Polizu, and L. Yahia. Accelerated fatigue behavior and mechano-physical characterizations of in vitro physiological simulation of nitinol stents. J. Appl. Biomater. Biomech. 5(2):117–124, 2007.
Scheinert, D., S. Scheinert, J. Sax, C. Piorkowski, S. Braunlich, M. Ulrich, G. Biamino, and A. Schmidt. Prevalence and clinical impact of stent fractures after femoropopliteal stenting. J. Am. Coll. Cardiol. 45(2):312–315, 2005.
Schillinger, M., S. Sabeti, P. Dick, et al. Sustained benefit at 2 years of primary femoropopliteal stenting compared with balloon angioplasty with optional stenting. Circulation 115:2745–2749, 2007.
Schillinger, M., S. Sabeti, C. Loewe, P. Dick, J. Amighi, W. Mlekusch, O. Schlager, M. Cejna, J. Lammer, and E. Minar. Balloon angioplasty versus implantation of nitinol stents in the superficial femoral artery. N. Engl. J. Med. 354(18):1879–1888, 2006.
Schneider, F., T. Fellner, J. Wilde, and U. Wallrabe. Mechanical properties of silicones for MEMS. J. Micromech. Microeng. 2008. doi:10.1088/0960-1317/18/6/065008.
Steegmueller, R., T. Fleckenstein, and A. Schuessler. Is Electropolishing Equal to Electropolishing? Proceedings from the Materials & Processes for Medical Devices Conference 2005, ASM 2006, pp. S.163–S.168.
Zeller, T. Current state of endovascular treatment of femoro-popliteal artery disease. Vasc. Med. 12(3):223–234, 2007.
Zhao, H. Q., A. Nikanorov, R. Virmani, R. Jones, E. Pacheco, and L. B. Schwartz. Late stent expansion and neointimal proliferation of oversized nitinol stents in peripheral arteries. Cardiovasc. Interv. Radiol. 32(4):720–726, 2009.
Acknowledgments
This work was carried out within the project ‘‘RT3S—Real Time Simulation for Safe vascular Stenting’’, partially funded by the European Commission under the 7th Framework Programme, GA FP7-2009-ICT-4-248801.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Ajit P. Yoganathan oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Meoli, A., Dordoni, E., Petrini, L. et al. Computational Modelling of In Vitro Set-Ups for Peripheral Self-Expanding Nitinol Stents: The Importance of Stent–Wall Interaction in the Assessment of the Fatigue Resistance. Cardiovasc Eng Tech 4, 474–484 (2013). https://doi.org/10.1007/s13239-013-0164-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-013-0164-4