Abstract
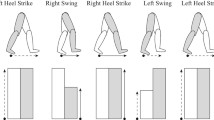
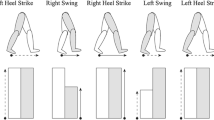
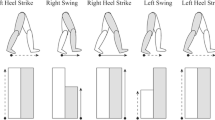
Gait rehabilitation after stroke often utilizes treadmill training delivered by either therapists or robotic devices. However, clinical results have shown no benefit from this modality when compared to usual care. On the contrary, results were inferior; perhaps, because in its present form it is not interactive and at least for stroke, central pattern generators at the spinal level do not appear to be the key to promote recovery. To enable gait therapy to be more effective, therapy must be interactive and visual feedback appears to be an important option to engage patients’ participation. In this study, we tested healthy subjects to see whether an implicit “visual feedback distortion” influences gait spatial pattern. Subjects were not aware of the visual distortion nor did they realize changes in their gait pattern. The visual feedback of step length symmetry was distorted so that subjects perceived their step length as being asymmetric during treadmill training. We found that a gradual distortion of visual feedback, without explicit knowledge of the manipulation, systematically modulated gait step length away from symmetry and that the visual distortion effect was robust even in the presence of cognitive load. This indicates that although the visual feedback display used in this study did not create a conscious and vivid sensation of self-motion (the properties of the optical flow), experimental modifications of visual information of subjects’ movement were found to cause implicit gait modulation. Nevertheless, our results indicate that modulation with visual distortion may require cognitive resources because during the distraction task, the amount of gait modulation was reduced. Our results suggest that a therapeutic program involving visual feedback distortion, in the context of gait rehabilitation, may provide an effective way to help subjects correct gait patterns, thereby improving the outcome of rehabilitation.





Similar content being viewed by others
References
Aagaard P (2003) Training-induced changes in neural function. Exerc Sport Sci Rev 31:61–67
Armstrong DM (1986) Supraspinal contributions to the initiation and control of locomotion in the cat. Prog Neurobiol 26:273–361
Bosecker C, Krebs HI (2009) MIT-Skywalker. In: International Conference on Rehabilitation Robotics. IEEE, Kyoto, Japan, pp 542–549
Brewer BR, Klatzky R, Matsuoka Y (2008) Visual feedback distortion in a robotic environment for hand rehabilitation. Brain Res Bull 75:804–813
Bronstein AM, Bunday KL, Reynolds R (2009) What the “broken escalator” phenomenon teaches us about balance. Ann NY Acad Sci 1164:82–88
Bussel B, Roby-Brami A, Neris OR, Yakovleff A (1996) Evidence for a spinal stepping generator in man. Electrophysiological study. Acta neurobiologiae experimentalis 56:465–468
Collins SH, Wisse M, Ruina A (2001) A three-dimensional passive-dynamic walking robot with two legs and knees. Int J Rob Res 20:607–615
Dietz V (2003) Spinal cord pattern generators for locomotion. Clin Neurophysiol: Off J Int Fed Clin Neurophysiol 114:1379–1389
Dietz V, Harkema SJ (2004) Locomotor activity in spinal cord-injured persons. J Appl Physiol 96:1954–1960
Duschau-Wicke A, von Zitzewitz J, Caprez A, Lunenburger L, Riener R (2010) Path control: a method for patient-cooperative robot-aided gait rehabilitation. IEEE Trans Neural Syst Rehabil Eng 18:38–48
Fouad K, Pearson K (2004) Restoring walking after spinal cord injury. Prog Neurobiol 73:107–126
Goldshmit Y, Lythgo N, Galea MP, Turnley AM (2008) Treadmill training after spinal cord hemisection in mice promotes axonal sprouting and synapse formation and improves motor recovery. J Neurotrauma 25:449–465
Hausdorff JM, Yogev G, Springer S, Simon ES, Giladi N (2005) Walking is more like catching than tapping: gait in the elderly as a complex cognitive task. Exp Brain Res 164:541–548
Hidler J, Nichols D, Pelliccio M, Brady K, Campbell DD, Kahn JH, Hornby TG (2009) Multicenter randomized clinical trial evaluating the effectiveness of the Lokomat in subacute stroke. Neurorehabil Neural Repair 23:5–13
Hornby TG, Campbell DD, Kahn JH, Demott T, Moore JL, Roth HR (2008) Enhanced gait-related improvements after therapist- versus robotic-assisted locomotor training in subjects with chronic stroke: a randomized controlled study. Stroke 39:1786–1792
Krebs HI, Volpe BT, Aisen ML, Hogan N (2000) Increasing productivity and quality of care: robot-aided neuro-rehabilitation. J Rehabil Res Dev 37:639–652
Lamontagne A, Fung J, McFadyen BJ, Faubert J (2007) Modulation of walking speed by changing optic flow in persons with stroke. J Neuroeng Rehabil 4:22
Malone LA, Bastian AJ (2010) Thinking about walking: effects of conscious correction versus distraction on locomotor adaptation. J Neurophysiol 103:1954–1962. doi:10.1152/jn.00832.2009
Pailhous J, Ferrandez AM, Fluckiger M, Baumberger B (1990) Unintentional modulations of human gait by optical flow. Behav Brain Res 38:275–281
Plummer P, Behrman AL, Duncan PW et al (2007) Effects of stroke severity and training duration on locomotor recovery after stroke: a pilot study. Neurorehabil Neural Repair 21:137–151
Prokop T, Schubert M, Berger W (1997) Visual influence on human locomotion. Modulation to changes in optic flow. Exp Brain Res 114:63–70
Rossignol S (1996) Visuomotor regulation of locomotion. Can J Physiol Pharmacol 74:418–425
Rossignol S, Dubuc R, Gossard JP (2006) Dynamic sensorimotor interactions in locomotion. Physiol Rev 86:89–154
Schmidt RA, Young DE (1991) Methodology for motor learning: a paradigm for kinematic feedback. J Mot Behav 23:13–24
Seif-Naraghi AH, Herman RM (1999) A novel method for locomotion training. J Head Trauma Rehabil 14:146–162
Shadmehr R, Smith MA, Krakauer JW (2010) Error correction, sensory prediction, and adaptation in motor control. Annu Rev Neurosci 33:89–108. doi:10.1146/annurev-neuro-060909-153135
Sheik-Nainar MA, Kaber DB (2007) The utility of a virtual reality locomotion interface for studying gait behavior. Hum Factors 49:696–709
Tseng YW, Diedrichsen J, Krakauer JW, Shadmehr R, Bastian AJ (2007) Sensory prediction errors drive cerebellum-dependent adaptation of reaching. J Neurophysiol 98:54–62. doi:10.1152/jn.00266.2007
Varraine E, Bonnard M, Pailhous J (2002) Interaction between different sensory cues in the control of human gait. Exp Brain Res 142:374–384
Werner C, Bardeleben A, Mauritz KH, Kirker S, Hesse S (2002) Treadmill training with partial body weight support and physiotherapy in stroke patients: a preliminary comparison. Eur J Neurol 9:639–644
Winstein CJ (1991) Knowledge of results and motor learning–implications for physical therapy. Phys Ther 71:140–149
Yogev G, Giladi N, Peretz C, Springer S, Simon ES, Hausdorff JM (2005) Dual tasking, gait rhythmicity, and Parkinson’s disease: which aspects of gait are attention demanding? Eur J Neurosci 22:1248–1256
Young DE, Schmidt RA (1992) Augmented kinematic feedback for motor learning. J Mot Behav 24:261–273
Acknowledgments
This work was supported in part by the Veterans Administration Baltimore Medical Center “Center of Excellence on Task-Oriented Exercise and Robotics in Neurological Diseases” B3688R. Dr. Krebs is a co-inventor in MIT-held patents for the robotic devices used to treat patients with neurological deficits. He holds equity positions in Interactive Motion Technologies, Inc., the company that manufactures this type of technology under license to MIT.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, SJ., Krebs, H.I. Effects of implicit visual feedback distortion on human gait. Exp Brain Res 218, 495–502 (2012). https://doi.org/10.1007/s00221-012-3044-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-012-3044-5