Abstract
Purpose
To evaluate heating efficacy of superparamagnetic iron oxide nanoparticles (SPIO) for electromagnetic ablation (EMA) of osteoid osteoma (OO) using an ex vivo model compared to radiofrequency ablation (RFA) and microwave ablation (MWA).
Methods
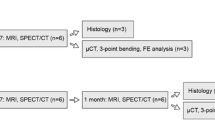
A model for OO using sliced bovine tibia and sliced muscle tissue was developed. A bone cavity filled with either a mixture of SPIO and agarose or pure agarose (control group) was established. EMA was performed using an experimental system, RFA and MWA using clinically approved systems, and the ablation protocols recommended by the vendor. For temperature measurements, fiberoptic temperature probes were inserted inside the cavity, on the outside of the periosteum, and at a 5 mm distance to the periosteum.
Results
Maximum temperatures with or without SPIO in the nidus were as follows: EMA: 79.9 ± 2.5/22.3 ± 0.7 °C; RFA: 95.1 ± 1.8/98.6 ± 0.9 °C; MWA: 85.1 ± 10.8/83.4 ± 9.62 °C. In RFA with or without SPIO significantly higher temperatures were achieved in the nidus compared to all other groups (p < 0.05). In MWA significantly higher temperatures were observed in the 5 mm distance to the periosteum compared to EMA and RFA with or without SPIO (p < 0.05). In MWA temperature decrease between nidus and the 5 mm distance to the periosteum was significantly lower than in RFA with or without SPIO (p < 0.0001). In MWA without SPIO temperature decrease was significantly lower than in the EMA group (p < 0.05).
Conclusion
In the experimental setting, ablation of OO is safe and effective using EMA. It is less invasive than RFA and MWA, and it theoretically allows repeated treatments without repeated punctures. In comparison, the highest temperatures in the nidus are reached using RFA.







Similar content being viewed by others
References
Eggel Y, Theumann N, Luthi F (2007) Intra-articular osteoid osteoma of the knee: clinical and therapeutical particularities. Joint Bone Spine 74:379–381
Greenspan A (1993) Benign bone-forming lesions: osteoma, osteoid osteoma, and osteoblastoma. Clinical, imaging, pathologic, and differential considerations. Skeletal Radiol 22:485–500
Cerase A, Priolo F (1998) Skeletal benign bone-forming lesions. Eur J Radiol 27(Suppl 1):S91–S97
Peyser A, Applbaum Y, Simanovsky N et al (2009) CT-guided radiofrequency ablation of pediatric osteoid osteoma utilizing a water-cooled tip. Ann Surg Oncol 16:2856–2861
Adam G, Keulers P, Vorwerk D et al (1995) The percutaneous CT-guided treatment of osteoid osteomas: a combined procedure with a biopsy drill and subsequent ethanol injection. Rofo 162:232–235
Fenichel I, Garniack A, Morag B et al (2006) Percutaneous CT-guided curettage of osteoid osteoma with histological confirmation: a retrospective study and review of the literature. Int Orthop 30:139–142
Gebauer B, Tunn PU, Gaffke G et al (2006) Osteoid osteoma: experience with laser- and radiofrequency-induced ablation. Cardiovasc Intervent Radiol 29:210–215
Rosenthal DI, Hornicek FJ, Torriani M et al (2003) Osteoid osteoma: percutaneous treatment with radiofrequency energy. Radiology 229:171–175
Skjeldal S, Lilleas F, Folleras G et al (2000) Real time MRI-guided excision and cryo-treatment of osteoid osteoma in os ischii—a case report. Acta Orthop Scand 71:637–638
Bruners P, Braunschweig T, Hodenius M et al (2010) Thermoablation of malignant kidney tumors using magnetic nanoparticles: an in vivo feasibility study in a rabbit model. Cardiovasc Intervent Radiol 33:127–134
Hilger I, Hergt R, Kaiser WA (2000) Effects of magnetic thermoablation in muscle tissue using iron oxide particles: an in vitro study. Invest Radiol 35:170–179
Johannsen M, Thiesen B, Wust P, Jordan A (2010) Magnetic nanoparticle hyperthermia for prostate cancer. Int J Hyperthermia 26:790–795
Jordan A, Scholz R, Maier-Hauff K et al (2006) The effect of thermotherapy using magnetic nanoparticles on rat malignant glioma. J Neurooncol 78:7–14
Mitsumori M, Hiraoka M, Shibata T et al (1996) Targeted hyperthermia using dextran magnetite complex: a new treatment modality for liver tumors. Hepatogastroenterology 43:1431–1437
Bitsch RG, Rupp R, Bernd L, Ludwig K (2006) Osteoid osteoma in an ex vivo animal model: temperature changes in surrounding soft tissue during CT-guided radiofrequency ablation. Radiology 238:107–112
Rosenthal DI, Alexander A, Rosenberg AE, Springfield D (1992) Ablation of osteoid osteomas with a percutaneously placed electrode: a new procedure. Radiology 183:29–33
Sans N, Galy-Fourcade D, Assoun J et al (1999) Osteoid osteoma: CT-guided percutaneous resection and follow-up in 38 patients. Radiology 212:687–692
Resnick RB, Jarolem KL, Sheskier SC et al (1995) Arthroscopic removal of an osteoid osteoma of the talus: a case report. Foot Ankle Int 16:212–215
Barei DP, Moreau G, Scarborough MT, Neel MD (2000) Percutaneous radiofrequency ablation of osteoid osteoma. Clin Orthop Relat Res 373:115–124
de Berg JC, Pattynama PM, Obermann WR et al (1995) Percutaneous computed-tomography-guided thermocoagulation for osteoid osteomas. Lancet 346(8971):350–351
Lindner NJ, Scarborough M, Ciccarelli JM, Enneking WF (1997) CT-controlled thermocoagulation of osteoid osteoma in comparison with traditional methods. Z Orthop Ihre Grenzgeb 135:522–527
Vanderschueren GM, Taminiau AH, Obermann WR, Bloem JL (2002) Osteoid osteoma: clinical results with thermocoagulation. Radiology 224:82–86
Woertler K, Vestring T, Boettner F et al (2001) Osteoid osteoma: CT-guided percutaneous radiofrequency ablation and follow-up in 47 patients. J Vasc Interv Radiol 12:717–722
Vanderschueren GM, Taminiau AH, Obermann WR et al (2004) Osteoid osteoma: factors for increased risk of unsuccessful thermal coagulation. Radiology 233:757–762
Hilger I, Andra W, Hergt R et al (2001) Electromagnetic heating of breast tumors in interventional radiology: in vitro and in vivo studies in human cadavers and mice. Radiology 218:570–575
Hilger I, Andra W, Bahring R et al (1997) Evaluation of temperature increase with different amounts of magnetite in liver tissue samples. Invest Radiol 32:705–712
Johannsen M, Gneveckow U, Thiesen B et al (2007) Thermotherapy of prostate cancer using magnetic nanoparticles: feasibility, imaging, and three-dimensional temperature distribution. Eur Urol 52:1653–1661
Organ LW (1976) Electrophysiologic principles of radiofrequency lesion making. Appl Neurophysiol 39:69–76
de Mercato G, Garcia-Sanchez FJ (1988) Dielectric properties of fluid-saturated bone: a comparison between diaphysis and epiphysis. Med Biol Eng Comput 26:313–316
Haemmerich D, Ozkan R, Tungjitkusolmun S et al (2002) Changes in electrical resistivity of swine liver after occlusion and postmortem. Med Biol Eng Comput 40:29–33
Skinner MG, Iizuka MN, Kolios MC, Sherar MD (1998) A theoretical comparison of energy sources—microwave, ultrasound and laser—for interstitial thermal therapy. Phys Med Biol 43:3535–35347
Simo KA, Tsirline VB, Sindram D et al (2013) Microwave ablation using 915-MHz and 2.45-GHz systems: what are the differences? HPB (Oxford) 15:991–996
Basile A, Failla G, Reforgiato A et al (2013) The use of microwaves ablation in the treatment of epiphyseal osteoid osteomas. Cardiovasc Intervent Radiol. doi:10.1007/s00270-013-0722-z
Salloum M, Ma RH, Weeks D, Zhu L et al (2008) Controlling nanoparticle delivery in magnetic nanoparticle hyperthermia for cancer treatment: experimental study in agarose gel. Int J Hyperthermia 24:337–345
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Isfort, P., Witte, H., Slabu, I. et al. Efficacy of Magnetic Thermoablation Using SPIO in the Treatment of Osteoid Osteoma in a Bovine Model Compared to Radiofrequency and Microwave Ablation. Cardiovasc Intervent Radiol 37, 1053–1061 (2014). https://doi.org/10.1007/s00270-013-0832-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-013-0832-7