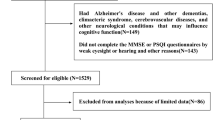
We compared the sleep quality indices between patients with mild cognitive impairment (MCI) and normal elderly subjects and analyzed the effects of sleep characteristics on cognitive functions. Cases of MCI patients (320 persons, MCI group) and 630 normal elderly with matched age, gender, and level of education (control group) were enrolled in this study. The Pittsburgh Sleep Quality Index (PSQI) was used to assess the sleep characteristics. The Mini-Mental State Examination (MMSE) and Montreal Cognitive Assessment (MoCA) were used to assess cognitive function. There were 110 (34.3 %) and 170 (27 %) cases with sleep disorders in the MCI and control groups, respectively (P < 0.01). There was a significant difference of total PQSI scores between the two groups, and the scores of sleep duration (factor III) and habitual sleep efficiency (factor IV) in the MCI group were significantly lower than those in the control group. Total PQSI scores negatively correlated with MoCA scores and MMSE scores. MoCA scores negatively correlated with scores of the sleep latency (factor II), sleep duration (factor III), and habitual sleep efficiency (factor IV), while MMSE scores negatively correlated with scores of factor III and factor IV. The scores of attention and calculation, reading and language understanding, and visuospatial function (MMSE), and also of visuospatial/executive function, attention, and clockdrawing test (MoCA) in MCI patients without sleep disorders were significantly higher than those in MCI patients with such disorders. The incidence of sleep disorders is higher in patients with MCI, compared with normal elderly. Effects of sleep disorders on cognitive functions are mainly reflected in the state of attention and visuospatial/executive function.
Similar content being viewed by others
References
S. Ancoli-Israel and L. Ayalon, “Diagnosis and treatment of sleep disorders in older adults,” Am. J. Geriat. Psychiat., 14, 95-103 (2006).
C. Stepnowsky and S. Ancoli-Israel, “Sleep and its disorders in seniors,” Sleep Med. Clin., 3, 281-293 (2008).
J. M. Ringman, L. D. Medina, Y. Rodriguez-Agudelo, et al., “Current concepts of mild cognitive impairment and their applicability to persons at risk for familial Alzheimer’s disease,” Current Alzheimer Res., 6, 341- 346 (2009).
M. Jelicic, H. Bosma, R. W. Ponds, et al., “Subjective sleep problems in later life as predictors of cognitive decline. Report from the Maastricht Ageing Study (MAAS),” Int. J. Geriat. Psychiat., 17, 73-77 (2002).
C. Sutter, J. Zöllig, M. Allemand, and M. Martin, “Sleep quality and cognitive function in healthy old age: the moderating role of subclinical depression,” Neuropsychology, 26, 768 -775 (2012).
S. M. Doran, H. P. Van Dongen, and D. F. Dinges, “Sustained attention performance during sleep deprivation: Evidence of state instability,” Arch. Ital. Biol., 139, 253-267 (2001).
H. P. Van Dongen, G. Maislin, J. M. Mullington, and D. F. Dinges, “The cumulative cost of additional wakefulness: Dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation,” Sleep, 26, 117- 126 (2003).
M. Thomas, H. Sing, G. Belenky, et al., “Neural basis of alertness and cognitive performance impairments during sleepiness. I. Effects of 24 h of sleep deprivation on waking human regional brain activity,” J. Sleep Res., 9, 335-352 (2000).
S. P. Drummond, A. Bischoff-Grethe, D. F. Dinges, et al., “The neural basis of the psychomotor vigilance task,” Sleep, 28, 1059-1068 (2005).
W. D. Killgore, A. P. Kendall, J. M. Richards, and S. A. McBride, “Lack of degradation in visuospatial perception of line orientation after one night of sleep loss,” Percept. Mot. Skills, 105, 276-286 (2007).
H. Babkoff, G. Zukerman, L. Fostick, and E. Ben- Artzi, “Effect of the diurnal rhythm and 24 h of sleep deprivation on dichotic temporal order judgment,” J. Sleep Res., 14, 7-15 (2005).
M. Haack, E. Lee, D. A. Cohen, and J. M. Mullington, “Activation of the prostaglandin system in response to sleep loss in healthy humans: Potential mediator of increased spontaneous pain,” Pain, 145, 136-141 (2009).
W. D. Killgore, and S. A. McBride, “Odor identification accuracy declines following 24 h of sleep deprivation,” J. Sleep Res., 25, 111-116 (2005).
R. C. Petersen, G. E. Smith, S. C. Waring, et al., “Mild cognitive impairment: clinical characterization and outcome,” Arch. Neurol., 56, 303-308 (1999).
Z. S. Nasreddine, N. A. Phillips, V. Bédirian, et al., “The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment,” J. Am. Geriat. Soc., 53, 695-699 (2005).
R. C. Petersen, “Mild cognitive impairment as a diagnostic entity,” J. Intern. Med., 256, 183-194 (2004).
D. J. Buysse, C. F. Reynolds, T. H. Monk, et al., “The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research,” Psychiat. Res., 28, 193-213 (1998).
D. J. Buysse, C. F. Reynolds 3rd, T. H. Monk, et al., “Quantification of subjective sleep quality in healthy elderly men and women using the Pittsburgh Sleep Quality Index (PSQI),” Sleep, 14, 331-338 (1991).
Y. L. Huang, R. Y. Liu, Q. S. Wang, et al., “Ageassociated difference in circadian sleep-wake and restactivity rhythms,” Physiol. Behav., 76, 597-603 (2002).
M. V. Vitiello and S. Borson, “Sleep disturbances in patients with Alzheimer’s disease: epidemiology, pathophysiology and treatment,” CNS Drugs, 15, 777- 796 (2001).
S. Gauthier, B. Reisberg, M. Zaudig, et al., “Mild cognitive impairment,” Lancet, 367, 1262-1270 (2006).
J. F. Gagnon, M. Vendette, R. B. Postuma, et al., “Mild cognitive impairment in rapid eye movement sleep behavior disorder and Parkinson’s disease,” Ann. Neurol., 66, 39-47 (2009).
D. L. Bliwise, “Sleep disorders in Alzheimer’s disease and other dementias,” Clin. Cornerstone, 6, S16-28 (2004).
C. E. Westerberg, E. M. Lundgren, S. M. Florczak, et al., “Sleep influences the severity of memory disruption in amnestic mild cognitive impairment: results from sleep self-assessment and continuous activity monitoring,” Alzheimer Dis. Assoc. Disord., 24, 325-333 (2010).
Y. Harrison, J. A. Horne, and A. Rothwell, “Prefrontal neuropsychological effects of sleep deprivation in young adults – a model for healthy aging?” Sleep, 23, 1067- 1073 (2000).
K. Jones and Y. Harrison, “Frontal lobe function, sleep loss and fragmented sleep,” Sleep Med. Rev., 5, 463-475 (2001).
W. D. Killgore, “Effects of sleep deprivation on cognition,” Prog. Brain Res., 185, 105-129 (2010).
A. R. Braun, T. J. Balkin, N. J. Wesenten, et al., “Regional cerebral blood flow throughout the sleep-wake cycle. An H2(15)O PET study,” Brain, 120, 1173-1197 (1997).
J. S. Durmer and D. F. Dinges, “Neurocognitive consequences of sleep deprivation,” Semin. Neurol., 25, 117-129 (2005).
R. D. Nebes, D. J. Buysse, E. M. Halligan, et al., “Self-reported sleep quality predicts poor cognitive performance in healthy older adults,” J. Geront. Psychol. Sci. Soc. Sci., 64, 180-187 (2009).
T. Manly, V. B. Dobler, C. M. Dodds, and M. A. George, “Rightward shift in spatial awareness with declining alertness,” Neuropsychology, 43, 1721-1728 (2005).
P. Lehmann, P. Eling, A. Kastrup, et al., “Self-reported sleep problems, but not fatigue, lead to decline in sustained attention in MS patients,” Mult. Scler., 19, 490-497 (2012).
S. J. Kass, J. C. Wallace, and S. J. Vodanovich, “Boredom proneness and sleep disorders as predictors of adult attention deficit scores,” J. Atten. Disord., 7, 83-91 (2003).
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
An, C., Yu, L., Wang, L. et al. Association Between Sleep Characteristics and Mild Cognitive Impairment in Elderly People. Neurophysiology 46, 88–94 (2014). https://doi.org/10.1007/s11062-014-9410-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11062-014-9410-0