Abstract
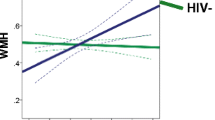
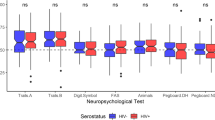
Our aim was to examine the clinical relevance of white matter hyperintensities (WMH) in HIV. We used an automated approach to quantify WMH volume in HIV seropositive (HIV+; n = 65) and HIV seronegative (HIV−; n = 29) adults over age 60. We compared WMH volumes between HIV+ and HIV− groups in cross-sectional and multiple time-point analyses. We also assessed correlations between WMH volumes and cardiovascular, HIV severity, cognitive scores, and diffusion tensor imaging variables. Serostatus groups did not differ in WMH volume, but HIV+ participants had less cerebral white matter (mean: 470.95 [43.24] vs. 497.63 [49.42] mL, p = 0.010). The distribution of WMH volume was skewed in HIV+ with a high proportion (23%) falling above the 95th percentile of WMH volume defined by the HIV− group. Serostatus groups had similar amount of WMH volume growth over time. Total WMH volume directly correlated with measures of hypertension and inversely correlated with measures of global cognition, particularly in executive functioning, and psychomotor speed. Greater WMH volume was associated with poorer brain integrity measured from diffusion tensor imaging (DTI) in the corpus callosum and sagittal stratum. In this group of HIV+ individuals over 60, WMH burden was associated with cardiovascular risk and both worse diffusion MRI and cognition. The median total burden did not differ by serostatus; however, a subset of HIV+ individuals had high WMH burden.


Similar content being viewed by others
References
Benjamini YHY (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc 57:289–300
Boone KB, Miller BL, Lesser IM, Mehringer CM, Hill-Gutierrez E, Goldberg MA, Berman NG (1992) Neuropsychological correlates of white-matter lesions in healthy elderly subjects. A threshold effect. Arch Neurol 49:549–554
Bornstein RA, Chakeres D, Brogan M, Nasrallah HA, Fass RJ, Para M, Whitacre C (1992) Magnetic resonance imaging of white matter lesions in HIV infection. J Neuropsychiatry Clin Neurosci 4:174–178
Chiao S, Rosen HJ, Nicolas K, Wendelken LA, Alcantar O, Rankin KP, Miller B, Valcour V (2013) Deficits in self-awareness impact the diagnosis of asymptomatic neurocognitive impairment in HIV. AIDS Res Hum Retrovir 29:949–956
De Guio F, Mangin JF, Duering M, Ropele S, Chabriat H, Jouvent E (2015) White matter edema at the early stage of cerebral autosomal-dominant arteriopathy with subcortical infarcts and leukoencephalopathy. Stroke 46:258–261
Debette S, Markus HS (2010) The clinical importance of white matter hyperintensities on brain magnetic resonance imaging: systematic review and meta-analysis. BMJ 341:c3666
Delis DC, Kramer JH, Kaplan E, Ober BA (2000) California Verbal Learning Test—second edition. Adult version. Manual Psychological Corporation, San Antonio
Fern RF, Matute C, Stys PK (2014) White matter injury: ischemic and nonischemic. Glia 62:1780–1789
Foley J, Ettenhofer M, Wright MJ, Siddiqi I, Choi M, Thames AD, Mason K, Castellon S, Hinkin CH (2010) Neurocognitive functioning in HIV-1 infection: effects of cerebrovascular risk factors and age. Clin Neuropsychol 24:265–285
Gutierrez J, Goldman J, Dwork AJ, Elkind MSV, Marshall RS, Morgello S (2015) Brain arterial remodeling contribution to nonembolic brain infarcts in patients with HIV. Neurology 85:1139–1145
Haddow LJ, Dudau C, Chandrashekar H, Cartledge JD, Hyare H, Miller RF, Jager HR (2014) Cross-sectional study of unexplained white matter lesions in HIV positive individuals undergoing brain magnetic resonance imaging. AIDS Patient Care STDs 28:341–349
Heaton RK (2004) Revised comprehensive norms for an expanded Halstead-Reitan battery: demographically adjusted neuropsychological norms for African American and Caucasian adults, professional manual. Psychological Assessment Resources, Lutz
Heaton RK, Grant I, Butters N, White DA, Kirson D, Atkinson JH, McCutchan JA, Taylor MJ, Kelly MD, Ellis RJ et al (1995) The HNRC 500—neuropsychology of HIV infection at different disease stages. HIV Neurobehavioral Research Center J Int Neuropsychol Soc 1:231–251
Heaton RK, Marcotte TD, Mindt MR, Sadek J, Moore DJ, Bentley H, McCutchan JA, Reicks C, Grant I, Group H (2004) The impact of HIV-associated neuropsychological impairment on everyday functioning. J Int Neuropsychol Soc 10:317–331
Ipser JC, Brown GG, Bischoff-Grethe A, Connolly CG, Ellis RJ, Heaton RK, Grant I, Translational Methamphetamine ARCG (2015) HIV infection is associated with attenuated frontostriatal intrinsic connectivity: a preliminary study. J Int Neuropsychol Soc 21:203–213
Islam MM, Topp L, Conigrave KM, Haber PS, White A, Day CA (2013) Sexually transmitted infections, sexual risk behaviours and perceived barriers to safe sex among drug users. Aust N Z J Public Health 37:311–315
Jahanshad N, Kochunov PV, Sprooten E, Mandl RC, Nichols TE, Almasy L, Blangero J, Brouwer RM, Curran JE, de Zubicaray GI, Duggirala R, Fox PT, Hong LE, Landman BA, Martin NG, McMahon KL, Medland SE, Mitchell BD, Olvera RL, Peterson CP, Starr JM, Sussmann JE, Toga AW, Wardlaw JM, Wright MJ, Hulshoff Pol HE, Bastin ME, McIntosh AM, Deary IJ, Thompson PM, Glahn DC (2013) Multi-site genetic analysis of diffusion images and voxelwise heritability analysis: a pilot project of the ENIGMA-DTI working group. NeuroImage 81:455–469
Jernigan TL, Archibald SL, Fennema-Notestine C, Taylor MJ, Theilmann RJ, Julaton MD, Notestine RJ, Wolfson T, Letendre SL, Ellis RJ, Heaton RK, Gamst AC, Franklin DR Jr, Clifford DB, Collier AC, Gelman BB, Marra C, McArthur JC, McCutchan JA, Morgello S, Simpson DM, Grant I, Group C (2011) Clinical factors related to brain structure in HIV: the CHARTER study. J Neurovirol 17:248–257
Kendall CE, Wong J, Taljaard M, Glazier RH, Hogg W, Younger J, Manuel DG (2014) A cross-sectional, population-based study measuring comorbidity among people living with HIV in Ontario. BMC Public Health 14:161
Kochunov P, Jahanshad N, Sprooten E, Nichols TE, Mandl RC, Almasy L, Booth T, Brouwer RM, Curran JE, de Zubicaray GI, Dimitrova R, Duggirala R, Fox PT, Hong LE, Landman BA, Lemaitre H, Lopez LM, Martin NG, McMahon KL, Mitchell BD, Olvera RL, Peterson CP, Starr JM, Sussmann JE, Toga AW, Wardlaw JM, Wright MJ, Wright SN, Bastin ME, McIntosh AM, Boomsma DI, Kahn RS, den Braber A, de Geus EJ, Deary IJ, Hulshoff Pol HE, Williamson DE, Blangero J, van’t Ent D, Thompson PM, Glahn DC (2014) Multi-site study of additive genetic effects on fractional anisotropy of cerebral white matter: comparing meta and megaanalytical approaches for data pooling. NeuroImage 95:136–150
Kramer JH, Jurik J, Sha SJ, Rankin KP, Rosen HJ, Johnson JK, Miller BL (2003) Distinctive neuropsychological patterns in frontotemporal dementia, semantic dementia, and Alzheimer disease. Cogn Behav Neurol 16:211–218
Maillard P, Fletcher E, Lockhart SN, Roach AE, Reed B, Mungas D, DeCarli C, Carmichael OT (2014) White matter hyperintensities and their penumbra lie along a continuum of injury in the aging brain. Stroke 45:1721–1726
Maniega SM, Valdes Hernandez MC, Clayden JD, Royle NA, Murray C, Morris Z, Aribisala BS, Gow AJ, Starr JM, Bastin ME, Deary IJ, Wardlaw JM (2015) White matter hyperintensities and normal-appearing white matter integrity in the aging brain. Neurobiol Aging 36:909–918
McArthur JC, Kumar AJ, Johnson DW, Selnes OA, Becker JT, Herman C, Cohen BA, Saah A (1990) Incidental white matter hyperintensities on magnetic resonance imaging in HIV-1 infection. Multicenter AIDS Cohort Study J Acquir Immune Defic Syndr 3:252–259
McMurtray A, Nakamoto B, Shikuma C, Valcour V (2007) Small-vessel vascular disease in human immunodeficiency virus infection: the Hawaii aging with HIV cohort study. Cerebrovasc Dis 24:236–241
McMurtray A, Nakamoto B, Shikuma C, Valcour V (2008) Cortical atrophy and white matter hyperintensities in HIV: the Hawaii Aging with HIV Cohort Study. J Stroke Cerebrovasc Dis 17:212–217
Morgan EE, Woods SP, Grant I, Group HIVNRP (2012) Intra-individual neurocognitive variability confers risk of dependence in activities of daily living among HIV-seropositive individuals without HIV-associated neurocognitive disorders. Arch Clin Neuropsychol 27:293–303
Morgello S, Murray J, Van Der Elst S, Byrd D (2014) HCV, but not HIV, is a risk factor for cerebral small vessel disease. Neurol Neuroimmunol Neuroinflamm 1:e27
Mortamais M, Portet F, Brickman AM, Provenzano FA, Muraskin J, Akbaraly TN, Berr C, Touchon J, Bonafe A, le Bars E, Menjot de Champfleur N, Maller JJ, Meslin C, Sabatier R, Ritchie K, Artero S (2014) Education modulates the impact of white matter lesions on the risk of mild cognitive impairment and dementia. Am J Geriatr Psychiatry 22:1336–1345
Nakamoto BK, Valcour VG, Kallianpur K, Liang CY, McMurtray A, Chow D, Kappenburg E, Shikuma CM (2011) Impact of cerebrovascular disease on cognitive function in HIV-infected patients. J Acquir Immune Defic Syndr 57:e66–e68
Nir TM, Jahanshad N, Busovaca E, Wendelken L, Nicolas K, Thompson PM, Valcour VG (2014) Mapping white matter integrity in elderly people with HIV. Hum Brain Mapp 35:975–992
Nyquist PA, Bilgel MS, Gottesman R, Yanek LR, Moy TF, Becker LC, Cuzzocreo J, Prince J, Yousem DM, Becker DM, Kral BG, Vaidya D (2014) Extreme deep white matter hyperintensity volumes are associated with African American race. Cerebrovasc Dis 37:244–250
Ovbiagele B, Saver JL (2006) Cerebral white matter hyperintensities on MRI: current concepts and therapeutic implications. Cerebrovasc Dis 22:83–90
Pfefferbaum A, Rosenbloom MJ, Rohlfing T, Kemper CA, Deresinski S, Sullivan EV (2009) Frontostriatal fiber bundle compromise in HIV infection without dementia. AIDS 23:1977–1985
Plessis SD, Vink M, Joska JA, Koutsilieri E, Stein DJ, Emsley R (2014) HIV infection and the fronto-striatal system: a systematic review and meta-analysis of fMRI studies. AIDS 28:803–811
Pomara N, Crandall DT, Choi SJ, Johnson G, Lim KO (2001) White matter abnormalities in HIV-1 infection: a diffusion tensor imaging study. Psychiatry Res 106:15–24
Schwarz C, Fletcher E, DeCarli C, Carmichael O (2009) Fully-automated white matter hyperintensity detection with anatomical prior knowledge and without FLAIR. Inf Process Med Imaging 21:239–251
Seider TR, Gongvatana A, Woods AJ, Chen H, Porges EC, Cummings T, Correia S, Tashima K, Cohen RA (2015) Age exacerbates HIV-associated white matter abnormalities. J Neurovirol
Shoamanesh A, Preis SR, Beiser AS, Vasan RS, Benjamin EJ, Kase CS, Wolf PA, DeCarli C, Romero JR, Seshadri S (2015) Inflammatory biomarkers, cerebral microbleeds, and small vessel disease: Framingham Heart Study. Neurology 84:825–832
Smith SM, Jenkinson M, Johansen-Berg H, Rueckert D, Nichols TE, Mackay CE, Watkins KE, Ciccarelli O, Cader MZ, Matthews PM, Behrens TE (2006) Tract-based spatial statistics: voxelwise analysis of multi-subject diffusion data. NeuroImage 31:1487–1505
Soontornniyomkij V, Umlauf A, Chung SA, Cochran ML, Soontornniyomkij B, Gouaux B, Toperoff W, Moore DJ, Masliah E, Ellis RJ, Grant I, Achim CL (2014) HIV protease inhibitor exposure predicts cerebral small vessel disease. AIDS 28:1297–1306
Su T, Wit FW, Caan MW, Schouten J, Prins M, Geurtsen GJ, Cole JH, Sharp DJ, Richard E, Reneman L (2016) White matter hyperintensities in relation to cognition in HIV-infected men with sustained suppressed viral load on cART. AIDS
Tustison NJ, Cook PA, Klein A, Song G, Das SR, Duda JT, Kandel BM, van Strien N, Stone JR, Gee JC, Avants BB (2014) Large-scale evaluation of ANTs and FreeSurfer cortical thickness measurements. NeuroImage 99:166–179
Weintraub S, Salmon D, Mercaldo N, Ferris S, Graff-Radford NR, Chui H, Cummings J, DeCarli C, Foster NL, Galasko D, Peskind E, Dietrich W, Beekly DL, Kukull WA, Morris JC (2009) The Alzheimer’s disease centers’ uniform data set (UDS): the neuropsychologic test battery. Alzheimer Dis Assoc Disord 23:91–101
Wright PW, Vaida FF, Fernandez RJ, Rutlin J, Price RW, Lee E, Peterson J, Fuchs D, Shimony JS, Robertson KR, Walter R, Meyerhoff DJ, Spudich S, Ances BM (2015) Cerebral white matter integrity during primary HIV infection. AIDS 29:433–442
Ylikoski A, Erkinjuntti T, Raininko R, Sarna S, Sulkava R, Tilvis R (1995) White matter hyperintensities on MRI in the neurologically nondiseased elderly. Analysis of cohorts of consecutive subjects aged 55 to 85 years living at home. Stroke 26:1171–1177
Yoshita M, Fletcher E, Harvey D, Ortega M, Martinez O, Mungas DM, Reed BR, DeCarli CS (2006) Extent and distribution of white matter hyperintensities in normal aging, MCI, and AD. Neurology 67:2192–2198
Acknowledgements
National Institutes of Health grants: K23-AG032872 (VV), P30 AG010129 (CD), K01 AG030514 (OC); The Larry L. Hillblom Foundation; the University of California, San Francisco/Gladstone Institute of Virology and Immunology Center For Acquired Immune Deficiency Syndrome Research; the University of California, San Francisco Acquired Immune Deficiency Syndrome Research Institute, K24MH098759 (VV) and P50-AG023501 (BM). Additional support from the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health, through the University of California, San Francisco-Clinical and Translational Science Institute Grant No. UL1 RR024131.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Valcour has served as a consultant for ViiV Healthcare and Merck related to aging and HIV. The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Watson, C., Busovaca, E., Foley, J.M. et al. White matter hyperintensities correlate to cognition and fiber tract integrity in older adults with HIV. J. Neurovirol. 23, 422–429 (2017). https://doi.org/10.1007/s13365-016-0509-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13365-016-0509-5